Bridging Silence: Systematic Hearing Care for Individuals with Intellectual Disabilities
- The Problem: Individuals with ID experience age-related hearing loss up to 30 years earlier, yet 74% of cases go undetected due to communication barriers.
- The Solution: Designed a collaborative "3+1" care model that empowers caregivers to conduct daily screenings while bringing professional on-site audiological and ENT interventions to the facilities.
- The Impact: Trained 44 caregivers, screened 129 individuals, successfully addressed critical hidden barriers (e.g., 50% severe cerumen impaction rate), and established a sustainable routine screening protocol.
The Challenge: Unheard Voices in ID Care
Individuals with Intellectual Disabilities (ID) face age-related hearing loss 10 to 30 years earlier[1] than the general public. Alarmingly, an estimated 74% of these cases go entirely undetected[2].
Because individuals with ID often struggle to express auditory discomfort, their hearing loss is frequently misdiagnosed as cognitive decline or behavioral issues. This invisible barrier not only diminishes their quality of life but also places an immense, hidden strain on their caregivers. My mission was to break this cycle by introducing a proactive, sustainable hearing care system into long-term care facilities.
Hearing care for the ID population isn't just about reading audiograms; it's about actively removing the physical and systemic barriers that silence them.
My Approach: The Collaborative "3+1" System
To bridge the critical gap between medical resources and long-term care institutions, I designed a collaborative "3+1" Modular System. This model divides responsibilities efficiently: the professional audiology team handles the core 3 phases (Training, Diagnostics, Rehab), empowering the facility caregivers to execute the vital "+1" phase (Routine Screening), creating a sustainable detection loop.
Core Clinical Pathway
Equipping frontline staff with basic knowledge and screening techniques.
On-site cerumen management and adaptive audiometry diagnostics.
Delivering personalized reports and introducing assistive tech.
Routine Screening
Empowered caregivers independently conduct the Hand Rub Hearing Screening in daily routines.
Clinical Execution & Key Discoveries
Executing this multi-year initiative (2024-2025) required continuous adaptation to the unique physiological and behavioral needs of the ID population. Here are the core insights and actions from the front lines:
Uncovering Hidden Physical Barriers
During our clinical assessments, I discovered an unexpectedly high rate of severe cerumen (earwax) impaction—affecting 50% of the evaluated cases. Due to irregular ear canal shapes and a lack of routine cleaning[3] , sound was physically blocked. I coordinated immediately with our ENT partners for specialized, on-site cerumen removal, instantly restoring baseline hearing for many individuals.
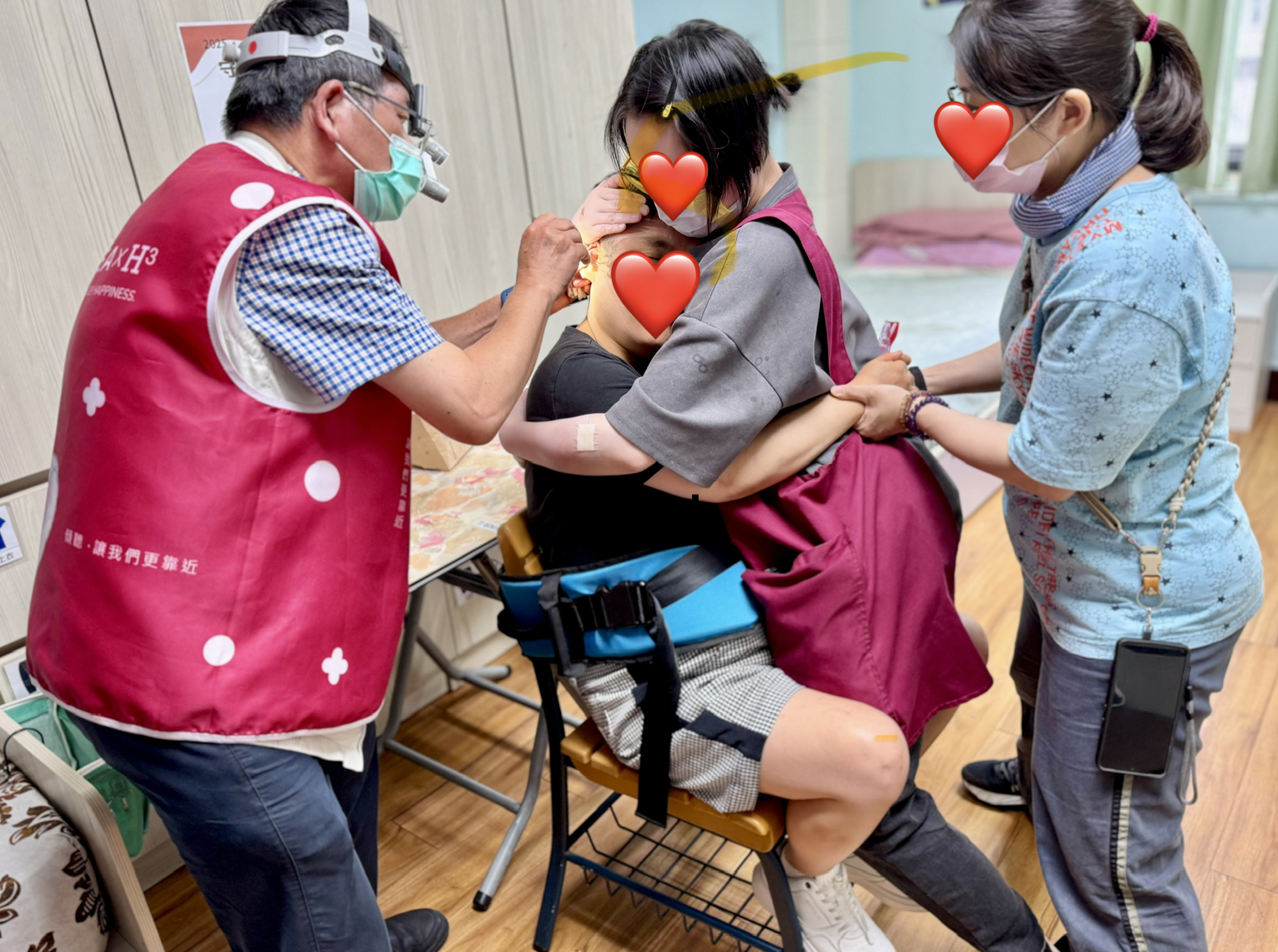
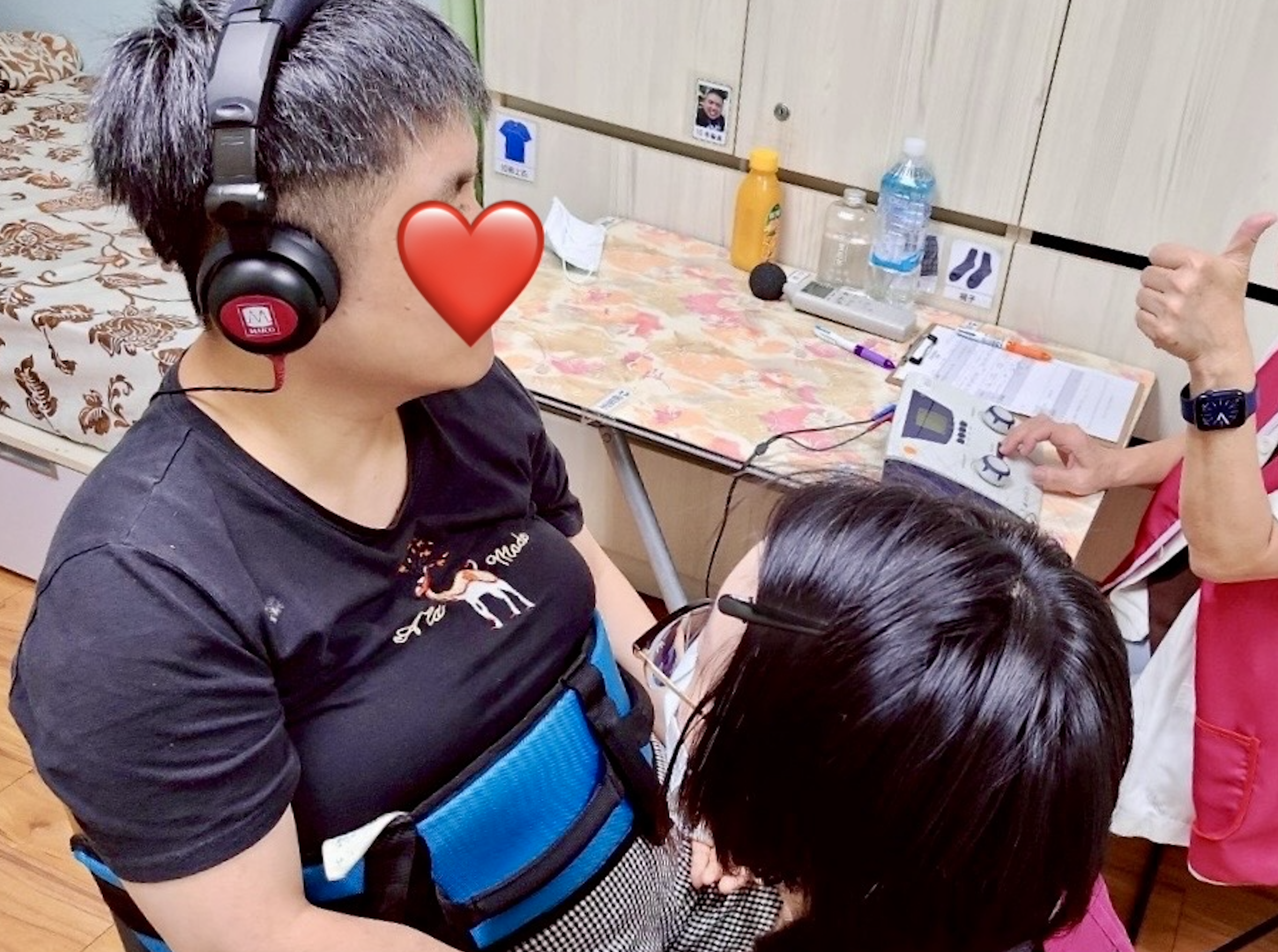
Adaptive Audiometry in Action
Traditional Pure Tone Audiometry (PTA) often fails with ID patients due to attention deficits. I successfully adapted testing protocols by incorporating behavioral observation audiometry (e.g., monitoring eye movements, clapping responses, or cessation of repetitive motions) alongside conditioned play, ensuring we obtained highly reliable hearing thresholds.
Bridging the Caregiver Confidence Gap
Pre-training evaluations showed that while caregivers cared deeply, they lacked the confidence to intervene. Through targeted workshops, we empowered 44 caregivers to conduct initial screenings. This successfully filtered the most at-risk cases (a 22% referral rate) directly to my clinical team for advanced diagnostics, creating a highly efficient referral loop.
Looking Forward: A Sustainable Future
Beyond immediate medical intervention, the ultimate goal was to leave the institutions with a sustainable framework. I established actionable, long-term protocols for the facilities, including:
Routine Screening Cadence
Instituted evidence-based screening schedules (every 1-3 years depending on age and syndrome type) to catch cognitive and hearing decline early.
Optimized Communication
Standardized "Face-to-Face" communication strategies, ensuring unobstructed visual cues to significantly reduce communication fatigue for patients and staff.
References
- Meuwese-Jongejeugd, A., et al. (2006). Prevalence of hearing loss in 1598 adults with an intellectual disability: Cross-sectional population based study. International Journal of Audiology, 45(11), 660-669.
- Hild, U., et al. (2008). High prevalence of hearing disorders at the Special Olympics indicate need to screen persons with intellectual disability. Journal of Intellectual Disability Research, 52(6), 520-528.
- Neumann, K., & Cravo, M. (2017). Guidelines for regular ear and hearing screening in people with an intellectual disability. Workshop presented at the 13th Congress of the European Federation of Audiology Societies (EFAS), Interlaken, Switzerland.