Mobile Service Audiology: Bridging the Gap in Indigenous Communities
- The Challenge: Elders in remote Indigenous communities face severe geographical barriers to hearing healthcare, leading to high device abandonment rates.
- The Solution: Initiated a Mobile Audiology Service providing on-site screenings, personalized in-home fittings, and culturally-adapted auditory training.
- The Impact: Successfully bypassed geographical barriers, restored community connections, and supported Indigenous language preservation.
A Holistic Ecosystem for Hearing Rehabilitation
To create sustainable impact, I conceptualized a dual-track service architecture anchoring our efforts in Cultural Health Centers and Home Visits.
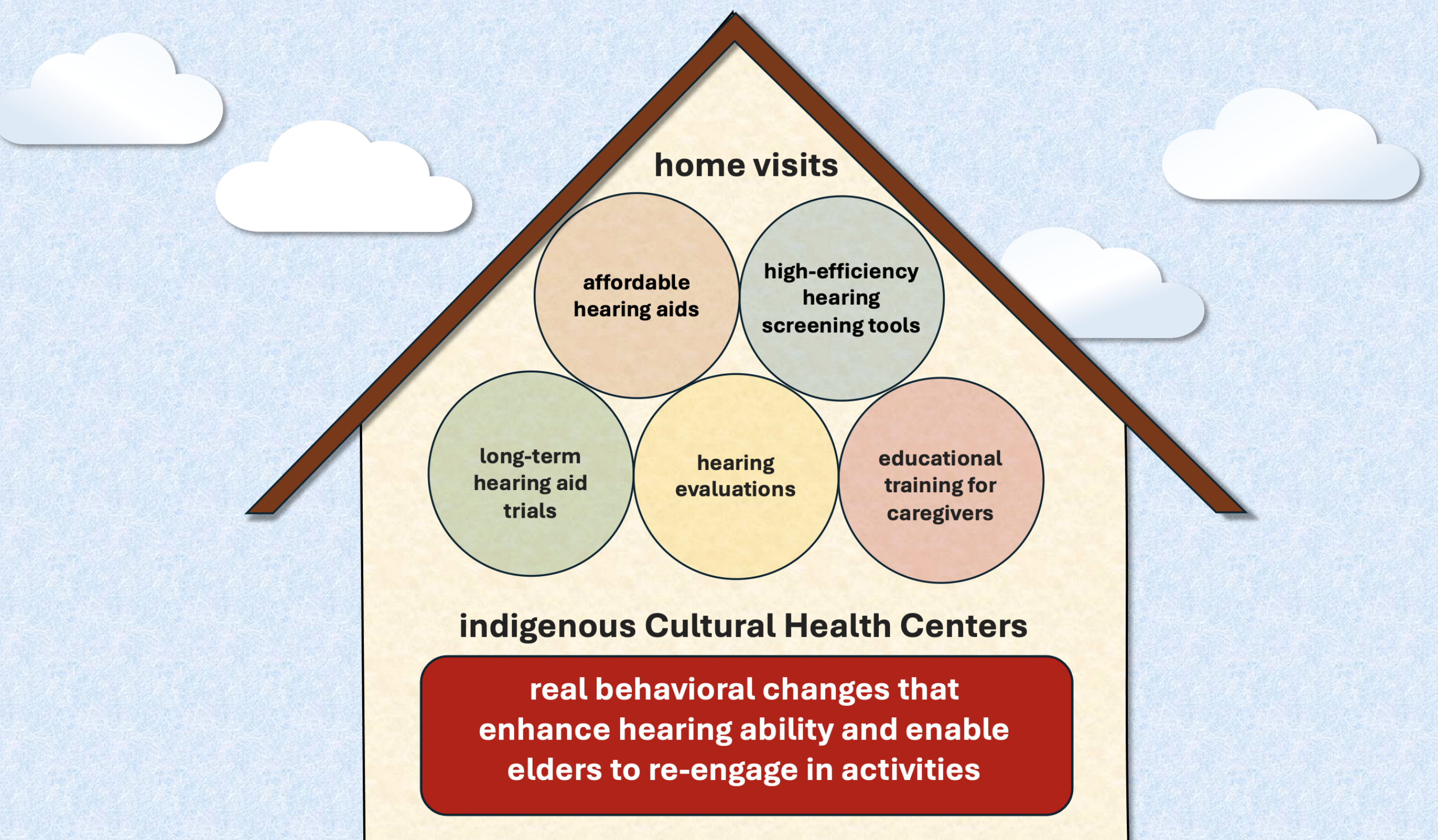
Taking Audiology into the Mountains
Instead of waiting for patients to navigate complex transportation systems to reach a city hospital, we packed our clinical expertise into mobile units. Collaborating with the Ruma Clinic, we established pop-up hearing care stations directly within Indigenous Cultural Health Centers.
By conducting home visits and on-site screenings, we observed the actual acoustic environments the elders live in. This crucial field insight allowed me to perform highly personalized hearing aid fittings that truly match their daily lifestyle needs, significantly reducing device abandonment rates.
Rehabilitation in Their Native Tongue
Providing a hearing aid is only the first step; rehabilitation dictates its success. I noticed that standard Mandarin auditory training materials often caused frustration and disengagement among Indigenous elders whose primary language is their native tongue.
To solve this, I spearheaded the design of localized hearing training tools tailored specifically to Indigenous languages. By using familiar words, environmental sounds, and cultural references, we transformed a frustrating medical task into an engaging, culturally respectful experience that elders eagerly participated in.
Redefining the Service Model
| Focus Area | Traditional Model | Our Mobile Service Model |
|---|---|---|
| Location | Distant city hospitals. | Pop-up stations in the community. |
| Device Fitting | Strictly quiet soundproof booth. | Personalized in-home fitting. |
| Rehabilitation | Standard Mandarin materials. | Localized training tools in native tongue. |
| Daily Support | Relies solely on family. | Caregivers are trained for maintenance. |
My Core Clinical Contributions
Education & Screening
Identified at-risk elders through screenings within community centers.
Home Testing & Fitting
Personalized programming matched to the elder's actual environment.
Culturally-Adapted Rehab
Planned and produced localized training tools in Indigenous languages.